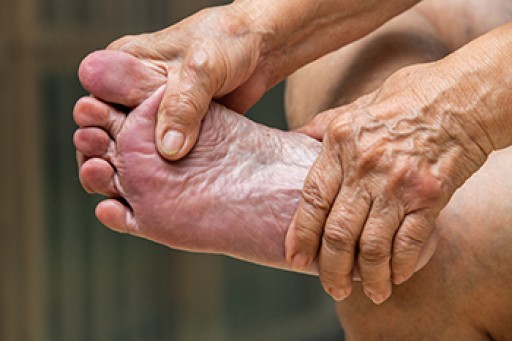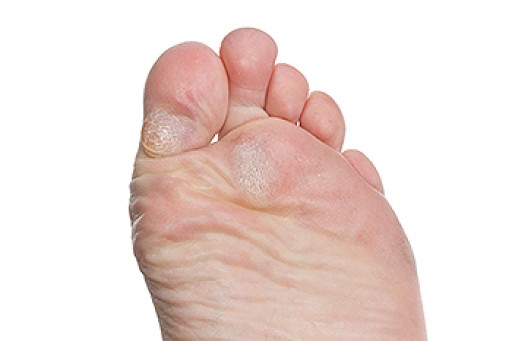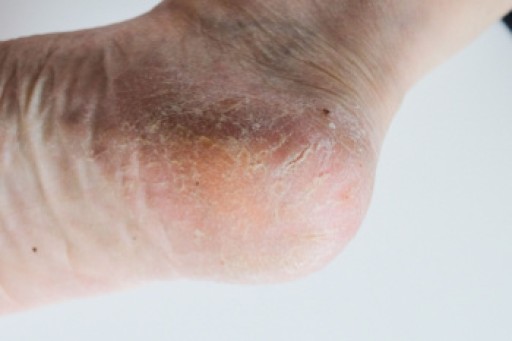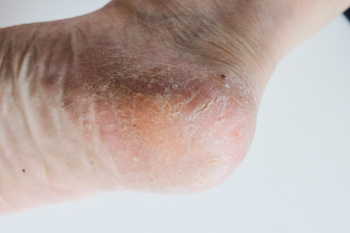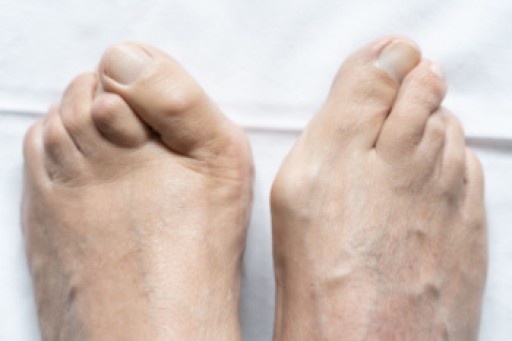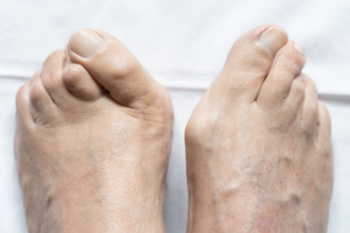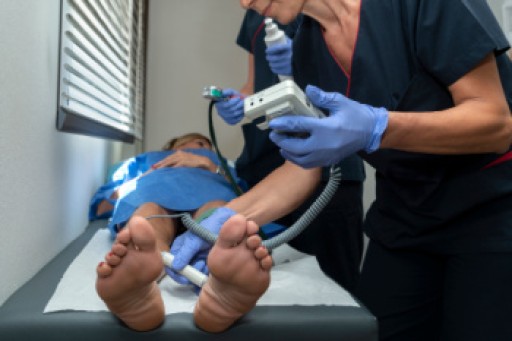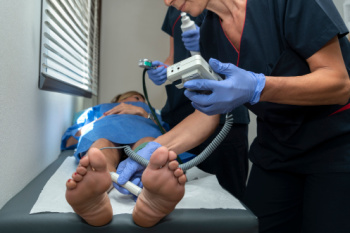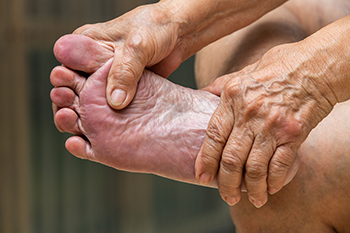
As the body ages, the fat pads on the feet undergo structural and functional changes that can affect comfort and mobility. Fat pad atrophy, a gradual thinning of the cushioning beneath the heel and forefoot, reduces shock absorption and increases sensitivity to pressure. The loss of elasticity in the skin and connective tissues further contributes to discomfort, making the feet more vulnerable to pain and injuries. Altered biomechanics, including changes in gait and posture, may develop as the body compensates for reduced cushioning. Increased pressure points can lead to calluses, soreness, and a higher risk of foot conditions. If you are elderly and have foot pain, it is suggested that you schedule an appointment with a podiatrist who can offer you effective relief methods.
If you need your feet checked, contact One of our Practitioner of Frankel foot & Ankle. Our practitioner will attend to all of your foot and ankle needs and provide you with quality treatment.
Geriatrics and Podiatry
When people age, some common issues that may occur are bone density loss, dry skin, poor circulation, and rough brittle nails. These issues may also affect your foot health if the necessary steps are not taken to alleviate the problems.
It is important to take care of your feet because feet that are injured or diseased can affect your overall health. Having painful feet hinders your ability to do daily activities or may decrease your willingness to do the things that you need to do.
Visiting Your Geriatrician
As we age, health problems become more likely, so it is essential to visit your doctor for check-ups to ensure that you are doing the best you can to take care of your health. It is recommended to check your feet frequently for any possible cuts, bruises, swelling, corns or any other irregularities.
Taking Care of Elderly Feet
Cracked or dry feet can be treated by applying moisturizer often. It is also important not to wear old socks because the older the sock is, the higher the possibility there will be that there is bacteria there. Wear fresh socks and make sure they fit properly.
Proper foot health means that you can have a more active lifestyle and you will not be bogged down by pain. Foot health also leads to good circulation, which is paramount for overall health.
If you have any questions, please feel free to contact our offices located in Milford, PA Middletown, NY Warwick, NY . We offer the newest diagnostic and treatment technologies for all your foot care needs.